 Skin cancer screening appointments can feel uncertain when you don’t know what to expect. Many people postpone or avoid these visits simply because they’re unfamiliar with the process, yet understanding what actually happens can ease those concerns. A typical screening involves more than a quick look at your skin. Your dermatologist will conduct a thorough examination, review your medical history, and assess any suspicious spots using specialized tools. The entire process is straightforward and designed to catch potential problems early. This guide walks you through each step of your appointment, from preparation to what happens if something concerning is discovered.
Skin cancer screening appointments can feel uncertain when you don’t know what to expect. Many people postpone or avoid these visits simply because they’re unfamiliar with the process, yet understanding what actually happens can ease those concerns. A typical screening involves more than a quick look at your skin. Your dermatologist will conduct a thorough examination, review your medical history, and assess any suspicious spots using specialized tools. The entire process is straightforward and designed to catch potential problems early. This guide walks you through each step of your appointment, from preparation to what happens if something concerning is discovered.
Who should get a skin cancer screening
More than 6 million adults receive treatment for skin cancer each year in the United States. While anyone can develop skin cancer, certain individuals face higher risks and benefit most from regular professional screenings.
Risk factors that increase your need for screening
Fair skin creates one of the most significant risk factors. People with lighter skin possess less melanin, which means reduced natural protection from UV rays. This increased vulnerability extends to those with blonde or red hair and blue, green, or light-colored eyes. Skin that burns or freckles easily compounds this risk further.
Your family’s medical history plays a crucial role in determining screening needs. If a close relative (parent, sibling, or child) has had skin cancer, your risk increases substantially. Having a family history of melanoma in two or more blood relatives warrants particular attention. Similarly, a personal history of melanoma or nonmelanoma skin cancers elevates your need for regular monitoring.
The number and type of moles on your body matter. Having many moles, particularly larger ones, raises melanoma risk. Atypical or dysplastic moles present additional concern on account of their irregular borders, varied colors, or asymmetrical appearance. Numerous actinic keratoses spots (gray or pink scaly patches in sun-exposed areas) also signal increased risk.
Sun exposure history directly impacts your screening needs. People who work outdoors regularly or spend significant recreational time in the sun face elevated risks. Previous sunburns, especially blistering ones, damage skin cells and increase cancer likelihood years later. Tanning bed use proves particularly dangerous. Indoor tanning before age 20 increases melanoma risk by nearly 50%, with each subsequent tanning session compounding the danger.
Age influences skin cancer development patterns. Most skin cancers occur in people over 50. However, melanoma represents one of the most common cancers in people under 30. People over 60 to 65, particularly those with light-colored hair and eyes, benefit significantly from annual screenings.
When to schedule your first appointment
Several medical organizations recommend starting professional skin cancer screenings at age 20 or older for average-risk individuals. The general guideline suggests skin examinations every three years between ages 20 and 40, then annually after 40. However, these recommendations apply only to people without concerning symptoms or elevated risk factors.
High-risk individuals need earlier and more frequent screenings. If you discover a first-degree relative has been diagnosed with skin cancer, schedule a baseline exam immediately, regardless of your age. An 18-year-old whose mother receives a melanoma diagnosis should get screened right away. Likewise, if you’ve had skin cancer previously, your children should undergo screening.
People with multiple risk factors require screenings at least once yearly, though some may need evaluations every three to six months. Those with a personal history of melanoma or multiple nonmelanoma skin cancers fall into this category. Monthly self-examinations become imperative for anyone with a history of skin cancer.
Low to average-risk individuals without family history or fair skin may only require professional exams once every one to two years. Nonetheless, monthly self-checks remain advisable for everyone to monitor new or changing moles.
Anyone noticing suspicious skin changes should seek evaluation immediately, even without traditional risk factors. The US Preventive Services Task Force notes insufficient evidence for routine total body screening in people without symptoms or risk factors. This makes awareness of your own skin particularly vital. Report any unusual moles, slow-healing spots, or sun-related skin changes to your doctor without delay.
What happens during your skin cancer screening appointment
Your appointment begins with administrative tasks. A dermatologist needs your complete medical history, including current medications and known allergies. Bring your medication list prepared, along with any dermatologic products you’ve been using. The provider will ask about personal or family history of skin cancer and any specific skin concerns you’ve noticed.
Medical history review and paperwork
During this initial discussion, your dermatologist will inquire about your risk factors and sun exposure history. If you’ve had previous skin screenings that resulted in biopsies, bring those records. This eliminates guesswork in understanding your risk level and helps avoid redundant procedures if you’ve had similar evaluations recently. Past biopsy results also inform treatment decisions if something suspicious appears.
Getting undressed and what to wear underneath
You’ll change into a medical exam gown in a private room. Most patients can keep their underwear on, though you’ll likely need to remove your bra. The extent of undressing depends on your comfort level and whether you have concerns in specific areas. If a spot on your genitalia worries you, you’ll be asked to remove underwear for that region. Correspondingly, the groin, buttocks, and genital areas receive examination only if you’re comfortable or express specific concerns about those locations.
The head-to-toe examination process
Your dermatologist examines every inch of skin, starting at the scalp and working downward to hands and feet. The inspection includes areas you rarely see yourself: behind your ears, between your toes and fingers, under fingernails and toenails, and across your back and buttocks. The provider keeps you covered with the gown, uncovering only one body section at a time. They’ll document the size, shape, color, and borders of each skin mark. This detailed record allows comparison during future annual exams, making it easier to detect changes over time.
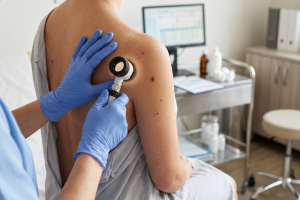
How dermatologists use a dermatoscope
When your doctor spots anything unusual or concerning, they’ll use a dermatoscope for closer inspection. This handheld magnifying device enlarges skin up to 10 times beyond what naked eyes can see [4]. The tool combines a flashlight and microscope, using polarized light to remove surface reflections that might obscure accurate diagnosis. Sometimes the dermatoscope hovers just above your skin to examine vascular changes, but usually it rests directly on your skin or nails to inspect moles, warts, and potential cancers. Just because your dermatologist uses this scope doesn’t signal cause for worry. In fact, most lesions examined prove benign. The device helps avoid unnecessary biopsies by definitively identifying harmless growths.
Duration of the appointment
A typical skin cancer screening takes 10 to 20 minutes. If you’ve never had atypical moles or skin cancer, expect the exam to last about 10 minutes. First-time visits run longer, as your doctor will discuss risk factors and gather comprehensive medical history. Appointments extend to 15 to 30 minutes when you have numerous moles requiring closer evaluation or a history of skin cancer warranting extra attention to high-risk body regions.
What your dermatologist is looking for
During your skin cancer screening, your dermatologist searches for three main types of skin cancer, each with distinct warning signs. Recognizing these patterns helps them distinguish cancerous growths from benign spots.
Basal cell carcinoma signs
Basal cell carcinoma most often appears on sun-exposed areas like your face, ears, neck, scalp, chest, shoulders, and back. Your dermatologist looks for a shiny, skin-colored bump that appears translucent or pearly white on lighter skin. On brown and Black skin, these bumps often look brown or glossy black. Tiny blood vessels may be visible within the bump, though they can be difficult to see on darker skin tones.
This cancer can also present as an open sore that bleeds, oozes, or crusts over, then appears to heal before returning. A reddish patch or irritated area that may crust, itch, or hurt signals another common presentation. Some basal cell carcinomas resemble a scar-like area that’s flat, white, yellow, or waxy with shiny, taut skin and poorly defined borders. A small pink growth with a slightly raised, rolled edge and a crusted indentation in the center may develop tiny surface blood vessels over time.
Squamous cell carcinoma signs
Squamous cell carcinoma typically develops on areas exposed to UV radiation, including your face, lips, ears, scalp, shoulders, neck, back of hands, and forearms. The skin around these growths usually shows sun damage like wrinkling, pigment changes, and loss of elasticity.
These cancers appear as thick, rough, scaly patches that may crust or bleed. They can resemble warts or open sores that don’t completely heal. Some show up as growths raised at the edges with a lower area in the center that may bleed or itch. A firm, dome-shaped growth with a raised border represents another common presentation. What looks like a scaly patch with broken skin can be squamous cell carcinoma in situ, the earliest form.
Melanoma and the ABCDE criteria
Your dermatologist uses the ABCDE criteria to evaluate suspicious moles. A stands for asymmetry, where one half of the mole doesn’t match the other. B represents border irregularity, with edges that are ragged, notched, or blurred. C means color that’s uneven, potentially including shades of brown, black, pink, red, white, or blue. D refers to diameter larger than 6 millimeters, about the size of a pencil eraser, though melanomas can be smaller. E indicates evolving, meaning the mole changes in size, shape, color, or develops new symptoms like bleeding, itching, or crusting.
Other skin changes and abnormalities
Dermatologists also watch for any new, changing, or unusual skin growths. Sores that fail to heal warrant attention. Spots that itch, bleed, or cause discomfort require closer inspection. Moles that suddenly grow larger or spread color from the edge into surrounding tissue raise concern.
If something suspicious is found
Finding an abnormal spot during your skin cancer screening triggers a specific next step: biopsy. This diagnostic procedure removes tissue for laboratory analysis, providing the only definitive way to confirm or rule out cancer.
The biopsy procedure explained
Your dermatologist selects from four biopsy techniques based on the lesion’s characteristics. A shave biopsy uses a sterile razor blade to remove the top layers of skin. Punch biopsy employs a circular tool to extract a deeper tissue core, ranging from 2 to 8 millimeters in size. Incisional biopsy removes part of a growth using a scalpel. Excisional biopsy cuts out the entire lesion, often recommended when melanoma is suspected.
The process begins with cleaning and numbing the area. Your provider injects lidocaine to eliminate pain, though you might feel a brief pinch from the needle. The actual biopsy takes about 15 minutes. Shave biopsies typically require no stitches, while punch and excisional biopsies may need one or two sutures to close the wound. Afterward, the provider applies antibiotic ointment and covers the site with a bandage. You can resume normal activities immediately.
Getting your results
Your tissue sample goes directly to a pathologist for microscopic examination. Results typically arrive within 7 to 10 days, though timing varies based on the laboratory’s workload, biopsy type, and case complexity. Weekends or holidays may extend this timeframe slightly.
The pathology report details whether the lesion is benign, precancerous, or malignant. It identifies the specific cell type involved, such as basal cell carcinoma, squamous cell carcinoma, or melanoma. The report also notes the depth and margins of abnormal cells, which guides treatment decisions.
Follow-up treatment options
Basal cell and squamous cell carcinomas can often be completely excised with a 4 to 6 millimeter margin of normal skin. Larger tumors, recurring growths, or those on high-risk sites like the nose, ears, and eyelids require the wider 6 millimeter margin. Many times, no additional treatment is needed beyond the initial excision.
Melanoma demands more extensive evaluation. If the biopsy reveals a thin melanoma (less than 0.75 millimeters thick), excision with at least a 5 millimeter margin suffices. Thicker melanomas require referral to a melanoma center for wider excision and potential sentinel lymph node removal. Squamous cell carcinoma also undergoes staging tests to determine if cancer has spread.
Recurrence monitoring becomes essential. Both basal cell and squamous cell carcinomas typically recur within 5 years of initial treatment if they return.
How to prepare for your appointment
Proper preparation ensures your dermatologist can perform a thorough examination without obstacles obscuring your skin.
What to skip before your visit
Come with clean, bare skin. Remove nail polish from fingers and toes, since skin cancers can form on nail beds. Skip makeup entirely or pack remover to use before your exam. Lotions, creams, oils, and fragrances should be avoided. Heavy hairspray makes scalp examination difficult. Wear your hair loose rather than in ponytails, buns, or clips. Remove jewelry before arriving.
What to bring with you
If you’ve had previous skin cancer biopsies, bring those records. They eliminate redundancy and help determine appropriate treatment if something suspicious appears. Bring your medication list, including prescriptions from other doctors. Show your dermatologist smartphone photos if you’ve documented spots changing over time. Create a written list of suspicious moles or areas that concern you. Making notes beforehand prevents forgetting important details during your appointment.
Questions to ask your dermatologist
Ask about your personal risk factors based on family history and sun exposure. Request guidance on monitoring moles yourself and which warning signs require follow-up. Inquire about sunscreen recommendations suited for your skin type. Correspondingly, ask how often you should return for future screenings based on your risk level.
Skin cancer screening appointments are straightforward procedures designed to catch problems early. The examination takes just 10 to 20 minutes, and knowing what to expect removes much of the uncertainty that keeps people from scheduling these vital checkups. As a matter of fact, preparation is simple: arrive with clean, bare skin and bring your medical history. Whether you fall into a high-risk category requiring annual screenings or need less frequent monitoring, regular professional examinations combined with monthly self-checks give you the best protection. Consequently, if you’ve been postponing your appointment, schedule it without delay. Early detection makes all the difference in successful treatment outcomes.
We Provide General Dermatology Services
We provide gentle, specialized care for children’s unique skin concerns, including birthmarks, eczema, acne, warts, and other pediatric dermatological conditions. Our friendly approach helps make these experiences positive for our youngest patients.
> Learn More
Contact Us (859) 283-1033 for a Consultation
—
 About Dermatology Associates of Northern Kentucky
About Dermatology Associates of Northern Kentucky
Dermatology Associates of Northern Kentucky offers a range of services for all age groups, including general and pediatric dermatology, dermatologic surgery, Mohs Micrographic surgery, laser and cosmetic procedures, and Dermatopathology.
> Learn More

 About Dermatology Associates of Northern Kentucky
About Dermatology Associates of Northern Kentucky